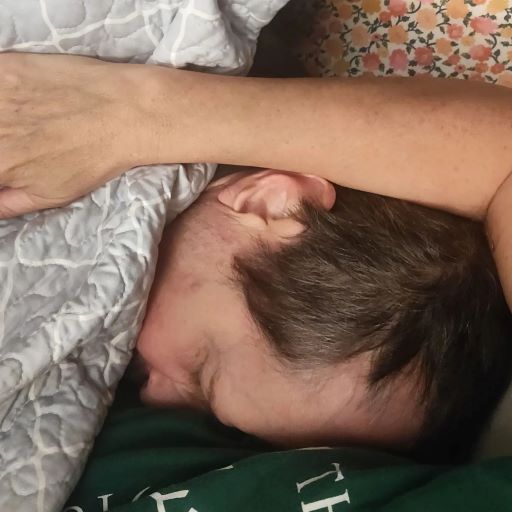
“What time is it?” Mark asked this afternoon, waking up from a nap. Two hours earlier, we had come home from a long morning at the hospital, where Mark had a Functional MRI scan.
“It’s two o’clock,” I said, glancing at the living room clock fully within his view.
“In the morning or afternoon?” he asked. The midday sun was hazy behind summer storm clouds.
“Afternoon,” I replied. “What time does it feel like to you?”
“7:30 in the afternoon.” He eyes were steadily holding mine.
“Ummm…there is no 7:30 in the afternoon,” I said, “There’s morning or evening.”
“There is a 7:30 in the afternoon,” he insisted.
“Okay. 7:30 is when you go to bed. Do you feel like it’s bedtime?”
“Yes.”
“Okay,” I said. “Do you want to go to bed?”
“Yes. ”
Mark shifted his weight and climbed into his wheelchair. He slowly pivoted and headed down the hallway. I waited until he passed the thermostat, then went back to check it. Mark is now changing the thermostat many times a day – every time he passes it – and always in a way that makes no sense. It was over 90℉ outside, and I had the air conditioning set to 78℉. He reset the thermostat to 71℉ and switched it from air conditioning to heat. After I adjusted it back, I followed him to our bedroom where he took off his sweatshirt because he was too warm.
“Good night,” he said.
“Night night,” I said. “You look handsome.”
“I am handsome,” he said, placing his hand on my arm and falling immediately asleep.
This is what life has been like – the wheelchair, increased confusion, disorientation – since a spate of seizures and a fall 10 days ago.
Weeks ago – three? Four? – Mark’s seizures ramped up, particularly while sleeping. I only recognized that he was having seizures because during his stay in the Epilepsy Monitoring Unit in March, I learned their particular clinical presentation. The kind of sleepytime twitches you and I might have – the startle of your arm or leg muscles, a quiver of the chin, the licking of your lips, a snorty snore – all can be evidence of Mark actively seizing. He started showing these signs frequently during naps and in the night. Sometimes they were fleeting but more so they started to persist, lasting 10, 20, 30 minutes.
If you have experience with seizures, you know that when a seizure lasts longer than five minutes, it can be considered a medical emergency. But what I also have learned is that Mark’s seizures are fairly out of control, and running to the ER everytime is useless. And we can’t live at the hospital. Mark is now considered to have status epilepticus. That’s when you have drug-resistant seizures that come and stay too long for their visit: a firework explosion of electricity in the brain that can create a chain reaction of other explosions. In Mark’s case, the seizures tend to start at a focal point in his left or right (but mostly left) frontal lobe. Where they go from there, and their severity and impact, can vary. The origin of the seizures is the radiation scarring (mostly) which, as Mark’s neurosurgeon said, is “fuel for seizures.”
In May, the medical board determined that Mark was not a candidate for brain surgery to scoop out the bad brain real estate. I was not disappointed to hear this. That surgery was a scary prospect, and I was not looking forward to the responsibility of deciding whether to proceed. Calling to give me that news, the epileptologist added a nighttime sedative to try to reduce Mark’s seizures. She said maybe there would be “a miracle,” and it would help.
I don’t know about you, but I am not a big fan of doctors talking about miracles.
The sedative did, actually, reduce Mark’s seizures for about a week. Then his seizures-while-sleeping resumed, and with a vengeance. Three, four nights a week, and often during his naps, I would watch and wonder what I should or could even do. I emailed the doctor for more ideas, more help. I picked up the prescription I had avoided buying – the epilepsy rescue nasal spray that costs $564 for a one month supply. This is a benzodiazepine, a tranquilizer and a scheduled drug. Essentially, if Mark’s brain was a raging fire, this was a bigger bucket of water to put it out. Mark was already on another benzo, and the pharmacist would not release the nasal spray to me until I explained why I was picking up a second one. (“Ask his doctor!” is what I wanted to say, but didn’t.)
When I got it home and read the teeny, tiny print on the medication, I found that the maximum you can give it is once every three days for a maximum of five doses per month.
My reaction was to laugh at the absurdity of this. The expense. The infrequency with which I could even give it to Mark.
Still, I waited until there was a night where I felt very, very confident that I was observing seizures, and then I sprayed it up Mark’s nose. Sure enough, the seizures stopped.
The problem was, the next night he had them again. So the medicine helped, but just for that single instance. Therefore, most days the seizures would keep propagating on their merry way while I could do nothing. How was that worth $564/month?
Ten days ago, I woke up at 1am to a thump and found Mark seizing on the floor in the dark hallway. He had gone through a good spell of making it through the night in bed, but had recently restarted his nighttime ramblings from bed to couch. He must have been making that journey when the seizure hit. He was conscious and was trying to stand up but his legs swayed like a landlubber at sea. I guided him down to the floor. After a few minutes, he wanted to try to stand, and again could not. After a while, we eventually made it to the couch.
The next morning, Mark’s left knee was the size of a cantaloupe and he could barely walk. A triangle of upper arm skin was hanging off. He was confused in a post-seizure way. He had fallen harder than I realized. Still, I decided to wait and see what was needed.
24 hours later, I decided it was the ER.
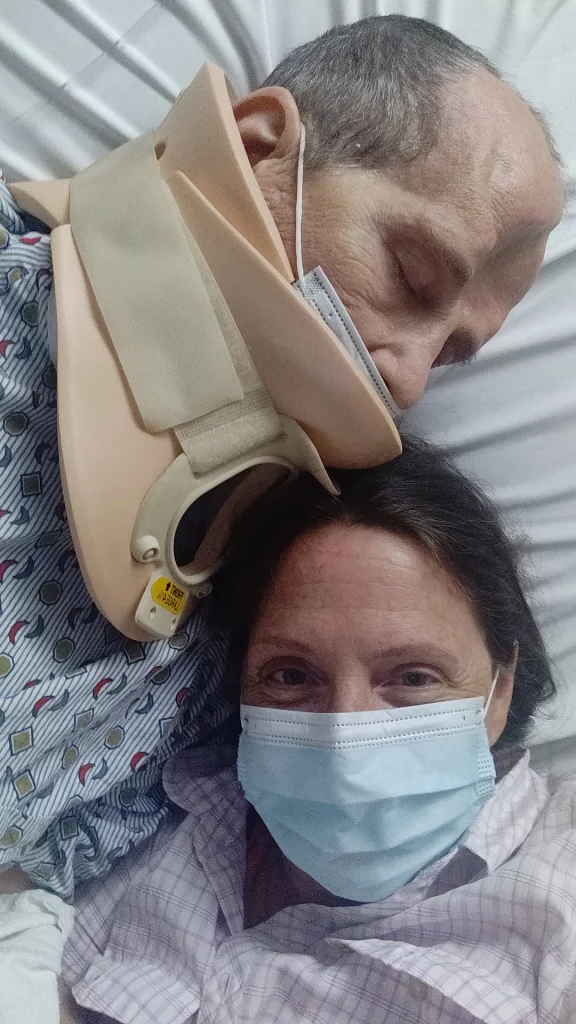
It was a zoo at Presby. The ER was full. The hospital was full. The waiting room was full. Gurneys lined the hallways. We were brought back for an assessment. “Mark had a seizure and fell and is not making sense and he doesn’t have all his skull,” was my run-on sentence that did the trick and got him an ER room. All true, of course, and yet I somehow still felt guilty.
Seven hours and xrays, CT scans, blood work and one cervical color later, everything came back okay. Nothing catastrophic had caused the seizure. No hidden brain tumor, no frightening blood levels. Nothing terrible resulted. No broken bones, they said, and no cerebral hemorrhage. Follow up with neuro and the PCP.
I began chasing the next steps. For the knee situation, I contacted Mark’s PT. “Which knee?” Phil asked. Of course, as things go, it’s the one that provided the tissue for his skull graft last year. Phil said based on Mark’s unique leg situation, to start with the plastic surgeon who performed that part of surgery. I contacted the plastic surgeon, who told me to start with an orthopaedic surgeon. The orthopaedic surgeon said to get an MRI. Which showed, contradictory to the x-ray, that Mark had fractured his kneecap. Fortunately, it was non-displaced. No surgery needed. Four to six weeks of no weight on it and keeping it straight in a brace, the ortho said.
For the brain problem, I contacted the epileptologist. She added a second dose of the sedative. “He’ll be more sleepy, but maybe that’s for the best.”
Since then, Mark has been what I’d call “out to lunch.” Maybe out to dinner and breakfast, too. This is either because the additional sedative is taxing him that much more, or because these seizures are taking, as his neurosurgeon said happens with seizures, “a cumulative toll.” The only way to discern which it is would be to reduce his seizure meds and see if his cognition improves, but that is a zero-sum game. It’s not worth the risk.
And thus, here we are. Over the course of a day or two, Mark changed in ways significant to his life and to ours. Matthew, who had gone to a national speech and debate competition in Louisville and missed this eventful week, came home to his dad back in a wheelchair, sleeping even more, and making very little sense. As usual, he and his brother took it in quietly. I continue to not really know how they integrate all this.
Mark now has very little short term memory. I can tell him three times between 7-8am what the morning holds, and by the time he’s in the car with me headed to an appointment or daycare, it’s gone. “Where are we going?” he asks. “The hospital,” I might say. “Why are we going there?” he responds.
Mark is being compliant about using his wheelchair, until he forgets why he is using it. I speak slowly, clearly, and loudly. “YOU BROKE YOUR KNEE CAP. YOU NEED TO NOT WALK FOR A MONTH SO THAT THE PIECES OF YOUR KNEE CAP STAY TOGETHER TO HEAL.” He looks at me blankly. “But I want to walk.” I explain again. “I’m going to walk,” he replies, hobbling to a standing position.
All I can do is hover in case disaster happens – another fall, which could hurt him in a myriad of ways including displacing that knee cap which would require surgery.
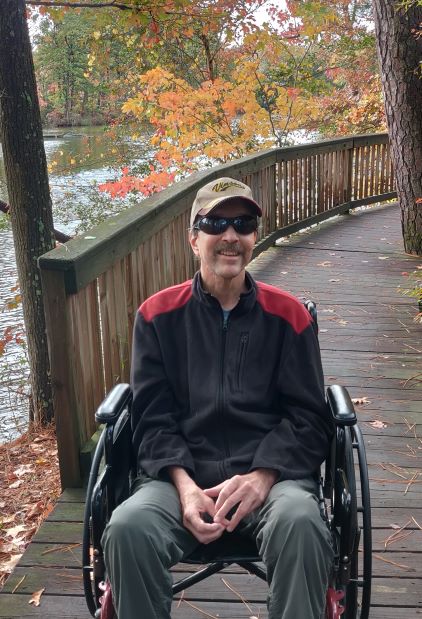
This is for sure a setback. Mark’s been working to recover use of this particular leg for an entire year. And while I was always fond of the safety the wheelchair provided amid the utterly chaotic feeling of everything being unsafe related to Mark, him riding around in it means he’s moving towards weakness rather than strength.
For now.
As Mark hates to hear me say, it is what it is.
Back to Mark’s brain for a moment. In the phone call where the epileptologist told me that brain surgery was off the table and that “a miracle” would be helpful, she said we were at a deadend for options. No medicines could stop the seizures, and this surgery was a no-go. We hung up. I had a very few minutes to process this news before she called me back, perky-voiced and with another idea. “You know, there’s a device that’s relatively new that can be implanted in the brain to detect and short circuit seizures. It’s sort of a pacemaker, but for the brain. Maybe that is a possibility.” She wondered if I was interested in exploring this.
It was about 5 o’clock, and I was talking to her from my back patio while watching a rose-breasted grosbeak at my feeder – my first time seeing one in my backyard. My elation at seeing the grosbeak collided with being flummoxed by her sudden change of plans. I mean, this was her field. Could she have thought about all the options before that first “there are no options” phone call? Having been through so much with Mark, though, this struck me as somehow predictably hilarious. “Sure!” I said, suppressing a gulp of laughter.
At some point, we will exhaust the options. For now, I continue to not be satisfied with letting Mark seize his way through the rest of his life. Not if there’s still a solution to consider. Mark is now in the queue to meet with an epilepsy neurosurgeon. That appointment is next week. Mark’s gotten all the scans needed for the doctor to make an informed decision about whether Mark is a surgical candidate. Meanwhile, I’ve done my homework. I’ve read copiously about radiation scarring, cluster seizures, drug resistant seizures, long term effects of seizures and long term effects of medications. I’ve watched educational videos, including one forty-minute surgical instruction video for the exact surgery for which Mark is being assessed. I do not recommend this video unless you are curious as to why I was really confused as to whether the instructor was using an actual severed head for his lesson. The modeling was very good. The drilling of boreholes was disturbing. The offhanded suggestion to the surgical residents to be careful not to tear the dura made a lot of sense.
I know, everyone. This is a lot. It is upsetting. I’m doing my best. I understood that we were in a nice run of time where things were stable. Stable-ish. I assumed they could not stay that way; that just does not seem to be the way Mark works, or the human body, or life. I’m taking it a day at a time, and I’m intimately familiar with that strategy. My world had grown a tiny bit for quite a few months, and I lived the heck out of that. Well, as much as I could. I could sit on the porch sometimes and trust Mark was okay inside. I did a little gardening. I had a few dinners out with friends. I took a lot of hikes and bike rides. Now I’m back to hovering, trusting the boys less with this big job (which is to keep the stress off them, not that they couldn’t do this) of caring for Mark. To compound things, this change in his status comes at the point at which I’m preparing to go back to work in a couple months, making planning all that more challenging. Let alone the emotional component.
I’ve been writing this in bed next to Mark. It’s now 5:30pm, and Mark still has his hand on my arm. He’s been showing signs of seizures for a while now, and I just made the decision to give him the last dose of the seizure rescue medicine that he can have this month. I don’t know whether it makes sense to buy it again. I don’t know whether Mark will sleep through the night or get up in an hour or two or five, unsteady and confused, needing support.
At this very moment, I promise that I feel okay even though things are really not okay. It is not easy, and that is not new. Is there a cumulative effect of all this on me? For sure. Somedays I feel it, and somewhere down the road I will reflect on it all more deeply. For now, I keep in mind Eckhart Tolle: “The present moment is all you ever have.” And I continue to navigate this path. I am thinking of an Ani DiFranco song:
…. both hands
Now use both hands
Oh, no don’t close your eyes
I am writing
Graffiti on your body
I am drawing the story of
How hard we tried
We keep going. I am holding onto tight. To me, and to Mark. With both hands.