The snow was bright and beckoning yesterday morning. I decided to prise myself off the couch and do something I haven’t done in a while; take Duppy for a walk. The luxury of the fenced-in yard had hit me fast when I moved to the deep ‘burbs, and while Duppy loves to run laps, she’s much more excited to hear the crinkle of plastic newspaper bags being pulled out of the closet and the word “walk.” Every tiny muscle in her body quivered as she tried her best to sit still while I pulled on my snow boots and got her into her harness.
We walked a few yards down the road before encountering a woman turning onto the street from a driveway. This house had sold in the fall — I hadn’t seen the new family yet. But from my station on the couch, I’ve seen this woman walking the neighborhood for the past few months. She’s not quite five feet tall, elderly, swathed in brightly patterned skirts and overskirts, always with a scarf wrapped around her head. I held Duppy back, taking care not to make this woman uncomfortable.
She slowed her pace: I slowed my pace. She took a couple steps toward me: I took a couple steps toward her. She made little walking-feet movements with her gloved fingers. She pointed up the hill. She made a looping motion. “Around the block?” I tried, “Yes, me too.” She made a circular motion with her hands that looked like the “shall we dance?” gesture ballet dancers make before a pas de deux. Yes, I nodded. She patted my arm. Together we began walking up the road.
She talked almost continually for the first part of our walk. I watched the smile lines around her eyes as she talked animatedly. I had no idea what she was saying. I caught the word Nepalese. She knew the word “good.” “My name is Diane,” I offered, patting my chest. She pulled her scarf aside and plucked at her shirt, smiling. I wasn’t sure if she thought the word for “shirt” in English was “diane.” She started to make medical-looking gestures. A needle in an arm? A lump in the belly? She talked and talked and pointed to her stomach. I worried that she was telling me she had cancer. Finally she made a cradling motion, and I understood that there’s a baby in her household.
We fell silent as we turned the corner at the top of the hill. Occasionally, I spoke just to put pleasant sounds in the air between us. Oh look, a bird. Hmm, the sky is so gray today. Isn’t the snow beautiful? She smiled back. Eventually she started pointing at my nose and laughing. Her face was hidden safely under her scarf. I knew mine must be turning red. She pointed at my cheeks and laughed more. I laughed back.
When we turned the final corner and reached her driveway, we stopped. She pointed to my nose and cheeks with concern. “I’ll go get warm,” I said. She made the pas de deux gesture. “Yes,” I said, “good.” “Good,” she said, and she walked back up her driveway.
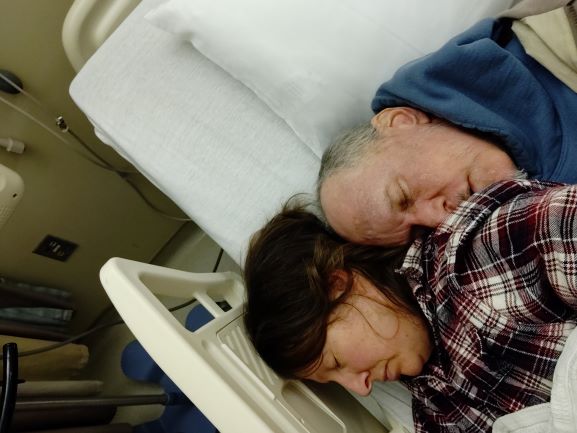
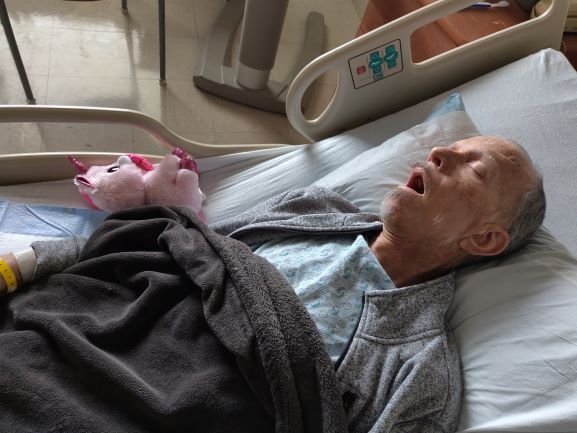
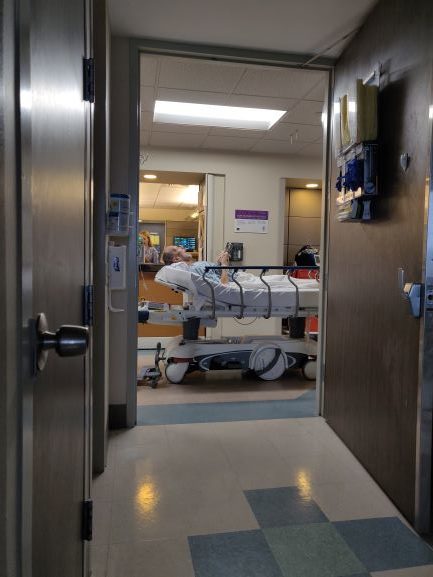
People bring up God a lot these days. Earlier this week, when Lizzy, Alma, Anya and I were sitting at the hospital with Mark, a rabbi came into the room. He introduced himself as a hospital chaplain. Apparently, when you engage palliative care, as I had, the chaplain comes with the package. I hadn’t realized. Over the course of the week, I had run into a kind, elderly Catholic chaplain. The first time, I was on the elevator with three women from the janitorial staff. When the chaplain got on, the women immediately bowed their heads. He blessed each of them, and then looked over at me. Sure, I said, I’ll take one. He laughed and blessed me, too.
Rabbi Perlman was new to me. He was relaxed and affable. He started by making small talk with Mark. “How are you feeling?” “Are you in pain?” Lizzy, Alma, Anya and I quietly studied our phones to give them the illusion of privacy as he arrived at “Do you have faith you’ll be healed?” and “Do you believe in God?”
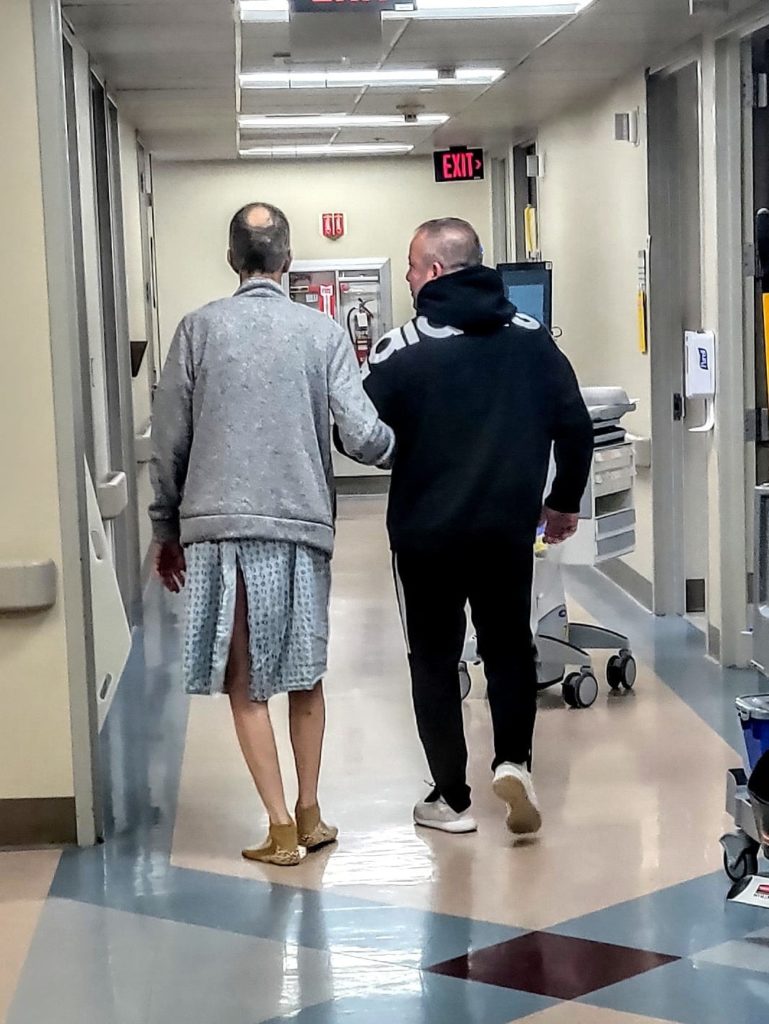
When a psychiatrist came to talk to Mark in the rehab on Friday, his opening line was “You’ve been through a lot. Do you feel like it’s been worth it?” Mark was sitting in his dysphagia group dining area, in a wheelchair with a bib, being spoon fed cream soup. He looked at the psychiatrist blankly. At least the rabbi had given some effort to ramp up to the heavy hitting questions, I thought.
It’s an inevitable part of this experience, this inquiry about how each of us is making sense of this. People look for finger- and footholds when they’re heading up a mountainside. Where we are is not a stopping place: we either have to find a way up or find a way down, and which is the safer route is up for debate.
Yet one thing I have always loved about Mark is his skill at living right here, in this moment. In part, this comes from having lived with his former wife’s cancer for six years. She was diagnosed before their third child was a year old. Two little boys, a baby, and cancer. Surgeries and treatments and remission leading only to more surgeries and more treatments and ultimately, suffering and death. Six years is a long time to ride a roller coaster and at some point, Mark figured out how to hop off. To live in each day only. It was a survival tactic. It’s one he’s kept. This has not always made him easy to live with. I’ve got a dose of East Coast in my blood. I’m a doer. I like goals and challenges. I’ve also got a dose of prairie in my blood, and I was attracted to Mark’s ability to take his time and let life expand rather than constantly kneading it. Yesterday when Mark was rejecting all the soft food lunch options — yogurt, pudding, soup, juice, cottage cheese, ice cream — I said, “What are we going to do, Mark?” He dryly replied, “Panic.” This has been his go-to response to me for years. Mark does not panic. He waits. He watches. He keeps doing what he’s doing until it’s clear to him that something else needs to be done.
The questions about meaning feel like they force something that doesn’t need to be forced. “What’s it gonna be? Now’s the time to choose.” Somehow, though, I don’t feel like we have to. There will be time to make meaning of it. To reflect and wonder. Don’t worry, people. Everyone involved has been baptized. We’re in it for the long haul, regardless of the fluctuations of the moment. I’m taking a page from Mark, and I am just living today.
I have had a lifetime of this question about God. Sometimes when something good happens, I quickly lob a thank you up to the sky. Sometimes when exceptional things come, I pause, wonder, and say thank you. When my kids were little, we had animals. We had lots of animals. Anya’s favorite pets were our bunnies. Anya had a beloved rabbit that she named Rascal, after reading Sterling North’s “Rascal” about a boy who raised a baby raccoon. We had a little outdoor pen that she could put the rabbit in, and one day she found the pen empty. Anya was beside herself. We all searched the yard, frantic to quell Anya’s fear. We looked and looked. Finally, Anya cried out, “That’s it! If we don’t find Rascal, I don’t believe in God anymore!” Then she ran down the sidewalk along the side of the house, tripped, and fell. As she lay there with her knee skinned, crying, she turned her head and there, behind a piece of wood leaning against the house, was Rascal. I wasn’t sure whether this was the Old Testament God smiting her, or the New Testament God having a great sense of humor. But all I could say was, thank you.
Yesterday, I immediately knew that the walk with my Nepalese neighbor was a gift. An exceptional gift. I had the company of someone with whom I was mutually delighted to be with, and who needed nothing from me other than my presence. The fact that I had nothing else to give did not matter.
And so I continually say thank you. I send the thanks up and out in all directions. For the rabbi for visiting. For Mark’s siblings who are so dedicated to loving us. For my school that has helped me have this time to take care of Mark. For my whole family prioritizing Mark. For Cathy from Louisiana who met me in Houston and hasn’t left my (Facebook) side. For Corinne who takes care of Mark’s kids like they are her own. For Mark’s friends who so clearly love him. For my friend Andrea who sends me one photo of natural beauty every day. For Hilary who always knows the right thing to say, which is often “I have no words.” For my friend Beth who gave me a key to her house, just so I know I have a place of respite. For so very many people, all of whom find their own way to be a part of our lives. I’m sending it up, out, and all around. Thank you.