Yesterday was difficult. I say that being a person who is not prone to hyperbole. Over the past seven months, I’ve listened to doctors describe Mark using words I’ve heard mostly in the context of geological sciences. It’s really my fault, because I ask a lot of questions. “How did you reattach the bone flap after you got the tumor out of his brain?” “We removed the bone flap by drilling bore holes, and we reattached it using titanium brackets at those locations.” And, “what is going on inside him that he’s bleeding from his nose and coughing out tissue-colored mucus?” “Due to the radiation and the cancer processes, his tissues are friable.”
Yesterday was difficult in a different way. I’d been at the hospital for 12 hours a day all week. My self-care had been going home to sleep at night, rather than sleeping in the pleather chair in Mark’s room. Not to boast, but I also took a shower every day. And ate food. Despite these excellent efforts to keep myself sane, I did manage to back into the garage door on Friday. And my underwear was on inside out. Still, I was proud of my little effort to keep myself going.
My brother Dale came to the hopsital at 8am so that I could sleep in. When I arrived at 10, Mark was more confused than on Friday. He’d only had one day of food after a week of nearly nothing, but still, I thought after being on continuous hydration, getting a unit of blood, and having a few IVs of magnesium, that he’d be returning to us a bit more by now. Dale arrived to Mark having pulled out his IV and refusing to let the nurse assistant clean him up.
Stubborn is in Mark’s general profile. They should have a check list at the top of the patient’s chart for baseline behaviors and attitudes. Mark giving the staff a hard time is annoying, but it’s also a sign of life. Check. He stayed stubborn all day yesterday. He didn’t want the nurses to help him back in bed. After they won that battle, I said to Mark, “What do you need?” “For the Nazis to go away.” “Can we end this part of the story where people are trying to control our lives?” Check.
Proud is also in Mark’s profile. And so it was difficult to see that Mark was in hospital briefs rather than his own undies, because Mark would never, ever allow that if he was aware of it. Uncheck. Anya, my oldest, was game for learning how to use Mark’s feeding tube. I taught her how to check his stomach for residual, flush the line, administer his dilantin, and then end with reflushing one more time. The fact that Mark allowed this without a word, silently watching TV, was completely out of character. Uncheck.
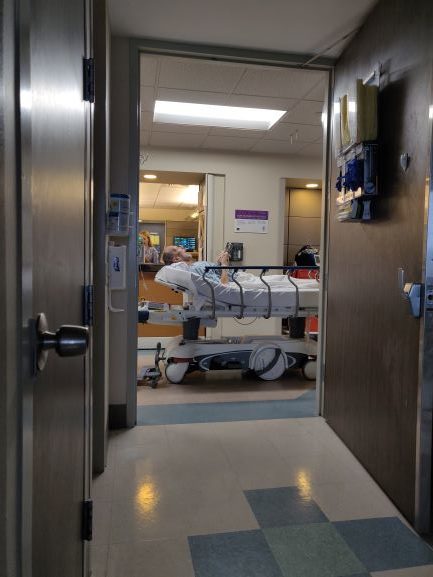
The crew of familiar oncology residents and doctors came in at 11:00. Mark would be discharged. His blood work looked okay, he was tolerating the feeding tube. I looked at them, and then at Mark, who was lying there slack-jawed, breathing loudly, staring straight ahead, not responding to anything around him. A 125 lb human machine that must be so strong despite being so weak; he just keeps going. “He is not at his baseline,” I said. I have learned the power of this word over the past months. “I don’t know how I’m going to get him to appointments, get him to the bathroom…” I’m sure I also looked like a human machine that is strong but weak, trying to keep running but reaching the fumes stage. They shuffled out.
A few minutes later, one doctor returned. They would call for a neuro oncology consult to get their opinion about what’s going on with Mark’s brain, and they called for a PT evaluation to see if Mark was safe to go home.
Part of what’s difficult for all caregivers is to have to realize and then exercise the power you have to advocate for the patient. There’s a comfort in thinking the doctors have this. You want them to be the quarterback who’s going to confidently throw the pass that wins the game. It is not a comfort to realize you really do have to be at bedside as much as possible to speak for the one who cannot. At the ER on Tuesday, I spoke to the oncologist who did not think a feeding tube was required yet. “He’s not eating anything. He’s not drinking anything. He has lost 42 pounds. He sleeps all the time. He’s exhausted.” The next morning, the oncology team decided a feeding tube would be merited. Today, the neuro oncology consult asked me what I mean when I say Mark is confused. I told the man, who was wearing a yarmulke, that Mark is referring to the nursing staff as Nazis. Not his baseline. Alma, my youngest, was there with me. We watched the doctor give Mark a rapid and thorough assessment. Memory, cognition, skeletal muscle function, vision. Mark passed some parts of the testing and failed others. “Generalized brain disfunction,” the doctor said. “Delirium, potentially caused by lack of nutrition. Could be inflammation from the radiation. The CT scan shows that there’s been no recent changes to the brain. Reimaging with MRI would not tell us anything about the impact of the radiation on the tumor. It’s too early post-treatment.” He said several thousand other words. It was hard to take it all in, even with two of use trying to hold onto the stream of information.
We waited for PT. Mark couldn’t form a clear thought. “What do you need?” I asked again. “Can we pull….can we….” he’d try. I went back to the basics: bathroom, water, blanket? Nothing. We’d both give up.
PT tried to get him out of bed. Mark was weak, unstable, confused, exhausted. He didn’t want to stand up. “Why not, Mr. Hrehocik?” “Because I’m losing control of everything,” he slurred. His mouth is bone dry. The radiation knocked out his saliva glands, and with his constant mouth-breathing, he’s hard to understand. The PT turned to me. How many stairs do we have in the house? Where is the bathroom? The list of questions was now familiar. The PT finished and said, “I’m recommending acute rehab. If we put together the need for PT, OT and speech therapy, he qualifies.” With all the fancy specialists attending to Mark, the PT had the power to say, no, this guy is not ready to go home.
The sense of relief was immediately followed by immense sadness. There is nothing Mark would rather do than go home, and I so want that for him, too. I have worked so hard to have him at home with us. I have months of training now of being on top of what he needs at all times. And now he needs more than we can give.
I gave birth to two children, Anya and Alma. I had natural childbirths, alert and aware and working hard to bring them into the world. It took many hours for each, and at the end their beautiful beings entered the room, one with a wail and one with quiet, wondering eyes. Sometimes I feel like a doula to Mark, trying to guide him back into our world. His journey is difficult, and the effort is immense. Sometimes he emerges for a few moments or a few hours, and then he retreats. We keep trying. We will keep trying.
My kids and I left the hospital last night at 6pm. One rode off on her motorcycle to her apartment. The other hopped into their own car to meet me back at the house. Tomorrow I will begin working with the hopsital to find an acute rehab placement for Mark. Another day. Difficult.
oooof. Like all the air just left the room. We knew Mark was really sick and then getting radiated and then not eating and not communicating well at all, but this? Oof. Somehow this was the worst, from my far-far-away perspective. I don’t know how you’re coping — how you have the strength to get out of bed, to stand up, and then shower love all over this dreadful situation. Much peace and continued strength to you, lovely. sbl
I remember this from Matt’s hospitalization. The doctors would come in, and sometimes it would be like the right hand did not know what the left hand was doing. Fortunately there was Dr. Howard, who was Matt’s hospitalist, and was supposed to know what everyone was doing. I also know this from being a hospital social worker. Sometimes the lower person on the totem pole is the wisest–of course as they are supporting the others. Let’s give PT a round of applause. You are Mark’s doula. It is exhausting, and there definitely are times when you just want somebody else to take charge. I remember you talking about wanting to hit the pause button and that was early on. Mark is lucky to have such a tenacious doula. 💕
Dear Dane. I keep reading. Praying and Thinking about the severe mercies that you live. The PT who saw Mark, saw you, and gave the sane word amidst all the specialists who didn’t know.
Id like your address so I can send you something. What do you need?
Love,
Petra
Thank you, friend. I’ll PM you.