The Big Surgery. That’s the shorthand I’ve been using for many months to describe this one. For almost a year, the neurosurgeon has been warning us that TBS might be in the cards. The craniotomy last August was not The Big Surgery. Neither was the one the August before. Or the one this past January.
“This is the ultimate fix,” the neurosurgeon has said repeatedly. “We know this will work, but it’s a very long surgery and has risks, so we want to try a different approach first.” That was last August. And then they unzipped Mark’s head and did the different approach first, in a surgery that lasted a dozen hours or so. And Mark has spent a year recovering from that.
So, this surgery is …. more complex? What’s more complex than unzipping someone’s head, removing their skull base, harvesting and installing in a tissue graft, ultimately adding some stomach fat to the graft, getting a CSF leak, and ending up with necrosis and part of your skull removed?
I mean, that seemed kinda big.
Free flap. That is the name of this procedure. The reason for it is this: the surgery in January did not actually do what they hoped. I’ve known that for a couple months now, in addition to knowing that at least one of the bad bacteria that Mark had to fight likely arrived through him being colonized in the hospital setting.
I found it too upsetting to talk about.
Since January’s surgery, I continue to visually monitor “the red spot” on Mark’s head. I email pictures to the neurosurgeon and write, “Should I worry now?” “How about now?” Not yet, he says. Keep monitoring. Keep sending pictures. Once, in early March, they brought him in for an MRI. The MRI did not show any new necrosis of his skull bone, which is GREAT NEWS, but it did show that the air pocket that they hoped would disappear from behind his forehead skin has not.
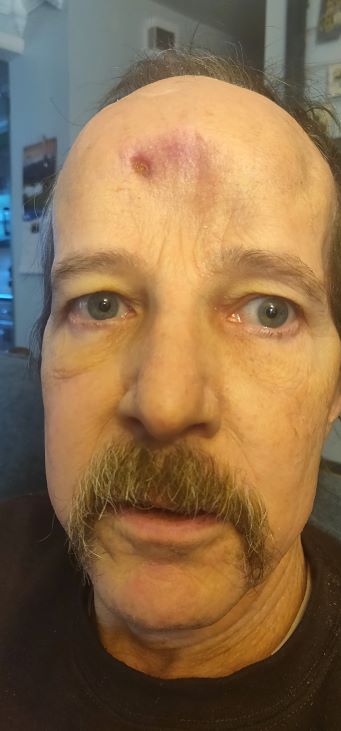
When you and I take a breath, the air goes into sinus pockets, which are surrounded by healthy bone tissue. When Mark takes a breath, the air goes up into his forehead and swirls around between the inside of his forehead skin and the repaired (and therefore “not normal” as the neurosurgeon says) lining of his brain. That’s how the bacteria established a front line up there in the first place. The goal of January’s surgery was to remove the dead tissue the bacteria was snacking on and have Mark’s forehead skin collapse against the lining of his brain. However, it didn’t collapse enough, despite the fact that if you look at Mark his forehead does look rather, you know, collapsed.
I thought I was only monitoring the red spot for fear of infection. Turns out, air isn’t too great, either.
“The path is clear… When you take a thin layer of skin and put air on both sides, it doesn’t survive…The tissue will eventually break down and there will be a draining area in the forehead…he will be left with a hole…nothing between the outside world and the lining of his brain…” These are my notes, scrawled on a piece of scrap paper during my phone call with the neurosurgeon.
“We need to fill in the dead space with something living,” he said.
He really is so very quotable.
The plan is to take vascularized tissue from Mark (thigh, perhaps) and sew it into place in “the dead space.” A plastics guy will meticulously sew all the blood vessels from the graft directly into blood supplies in Mark’s head. Then Mark’s forehead skin will have a nice place to rest right against a healthy piece of tissue being fed by a healthy blood supply, right next to Mark’s brain lining.
Like a life-sustaining tissue sandwich.
Mark doesn’t really know this yet. He knows that they want to discuss a surgery to solve the problem of the air pocket and the potential for infection. He doesn’t know it’s a 14 hour surgery, with multiple sites for wound repair, a recovery on some scale of those he’s had before, with all the risks inherent in any surgery let alone surgery on Mark. I think we have time to let this slowly unfold. The surgeon said he thinks we should do this within the next handful of months.
None of this is great news. We’ve just had the longest stretch of time since June 2019 without medical interventions being our primary hobby. Our days are comfortable. We spend a lot of time together. One day recently, I said, “We had a lot of adventures yesterday!” We had gone to Aldi and then stopped at Starbucks to pick up a coffee. “We sat on the front porch, too,” Mark said, without an ounce of irony.
Yes, yes we did. And that is much more than we typically do.
Last week, Mark and I went out to lunch. We both have had our vaccinations, and it felt okay to try. “You know,” I said, “I think you have become a different kind of partner to me. Not only a friend, not only a best friend, not only a husband. I feel more integrated with you. Like we are one.” “I feel the same,” he said. “When we are sitting on the couch together at night, there is nowhere I’d rather be.”
He was having a good brain day. The week before, he had tried to cook perogies in the cast iron skillet while they were still in their plastic bags.
I’m reluctant to give Mark back to the medical world. I have some sense of control right now. I know it’s an illusion.
Back in the day, in the long hallways at O’Hare Airport there was an otherworldly voice piped in above the people-mover conveyor belts. “Keep walking … Keep walking” the voice repeated. As I would reach the end of a stretch of conveyor belt, I would attempt to hop off while somewhat graciously maintaining my stride. Then I’d walked a bit to the next belt and leap on for another ride.
It’s the only way to keep going.
Thanks for making it clear what needs to be done. It’s a hard road to travel. Praying for you all.❤️🙏❤️🙏❤️
Thank you. Hard road, indeed. Love.
A little like ground hog day. Keeping you all in my thoughts.
Yep. Yep. Yep.